Latest
New study explains how Adenoviral COVID-19 vaccines trigger rare blood-clotting disorder
Published
2 months agoon
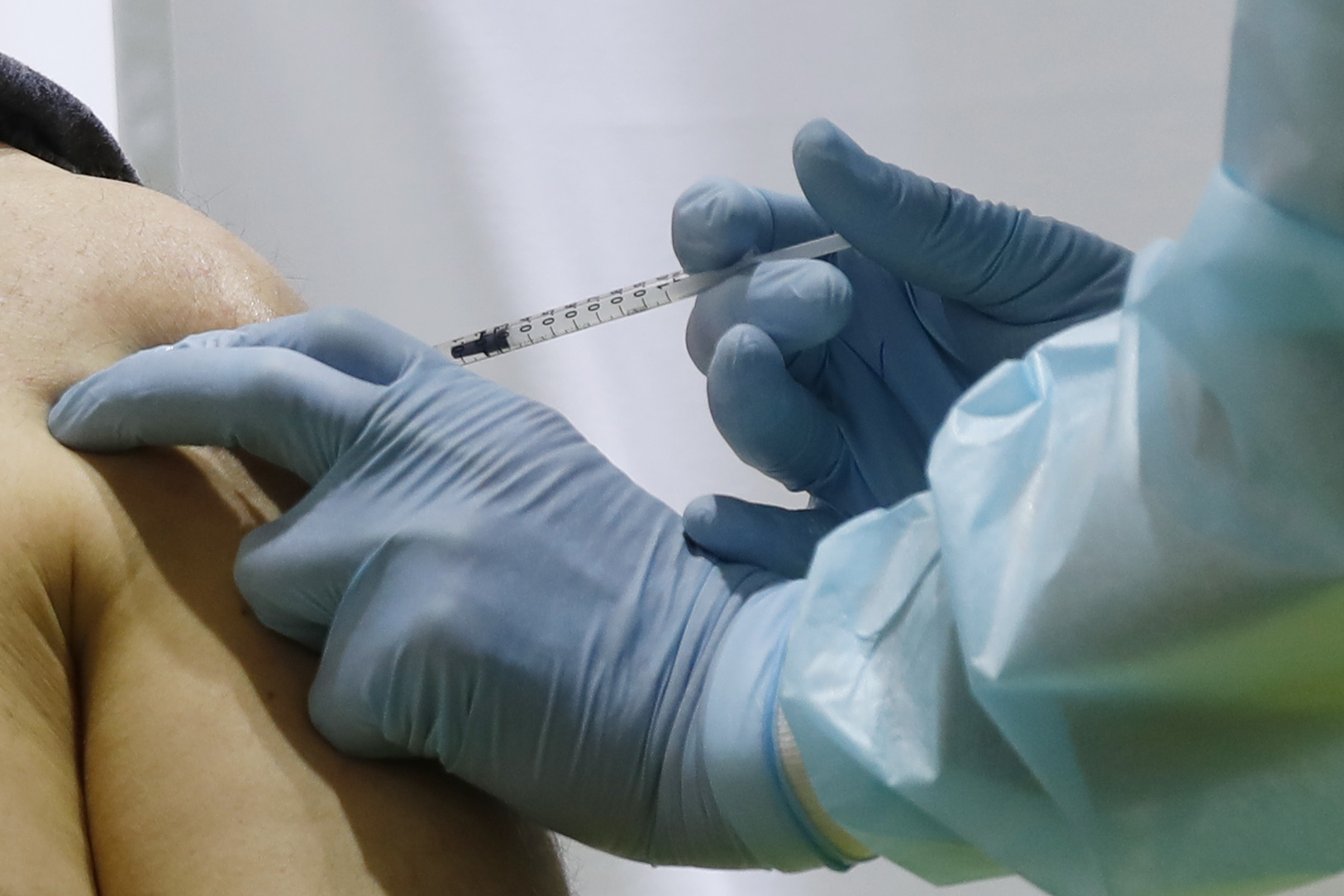
A new peer-reviewed study has shed light on how the AstraZeneca COVID-19 vaccine and the Johnson & Johnson COVID-19 vaccine can, in rare cases, lead to a serious blood-clotting condition known as vaccine-induced immune thrombocytopenia and thrombosis (VITT).
The findings, published last week in the New England Journal of Medicine, identify an immune mechanism linked to the adenoviral vector used in both vaccines.
Researchers found that in very uncommon instances, the body’s immune response to the adenovirus can mistakenly target its own platelets, triggering dangerous clot formation.
VITT is characterized by thrombosis — the formation of blood clots, often in the brain or abdomen — combined with thrombocytopenia, a condition marked by abnormally low platelet levels that can lead to uncontrolled bleeding. According to estimates cited in the study, approximately one in 200,000 recipients of the AstraZeneca or J&J vaccines developed VITT.
Both vaccines use an adenoviral vector to deliver genetic instructions for the SARS-CoV-2 spike protein into human cells, prompting an immune response against COVID-19. However, the study suggests that in rare cases, the immune system may confuse a normal adenovirus protein with platelet factor 4 (PF4), a human blood protein involved in clotting.
This phenomenon — known as molecular mimicry — causes the immune system to attack platelets, leading to clot formation and reduced platelet counts.
The study’s lead author, Dr. Ted Warkentin, professor emeritus of pathology and molecular medicine at McMaster University in Canada, said his team analyzed blood samples from 100 patients who developed VITT after receiving either vaccine.
All patients shared a specific gene variant common in roughly 60% of people of European descent. Some participants also had evidence of prior adenovirus infection, which typically causes mild cold-like symptoms and has previously been linked, in rare cases, to similar clotting disorders.
Warkentin noted that the research uncovers a previously unrecognized immune mechanism. He added that similar processes involving somatic mutations in antibody-producing cells could potentially explain other rare vaccine-related adverse events.
READ ALSO: Moderna COVID-19 shot posed higher heart inflammation risk for young men–Study
In a 2024 paper, the same research team had already concluded that the adenovirus vector itself was responsible for triggering VITT.
The findings have sparked renewed debate about vaccine safety and platform technologies.
Brian Hooker, chief scientific officer of Children’s Health Defense (CHD), said the study underscores the risks of treating vaccination as a “one-size-fits-all” intervention, arguing that genetic differences can have serious consequences.
Immunologist Jessica Rose, writing on Substack, described the mechanism outlined in the study as a “valid” explanation for VITT and suggested such risks should have been detected during clinical trials.
The AstraZeneca vaccine was never authorized in the United States but was widely used in Europe and other regions before several countries suspended or limited its use due to clotting concerns. In 2024, AstraZeneca discontinued production of its COVID-19 shot.
A class-action lawsuit in the United Kingdom alleges that the vaccine caused deaths and injuries, including cases of VITT.
The United States and other nations also halted use of the Johnson & Johnson vaccine following reports of rare clotting events.
After adenoviral vector vaccines were withdrawn or limited, mRNA vaccines produced by Pfizer and Moderna became dominant globally.
While some studies and case reports have described rare clotting events following mRNA vaccination — including a 2023 case report published in the journal Vaccines (Basel) — Warkentin emphasized that his team found no direct role for the spike protein in triggering VITT in their patients. Because mRNA vaccines do not contain adenovirus proteins, he said, the clotting mechanism described in the study would not apply to them.
However, other experts dispute that conclusion. Cardiologist Dr. Peter McCullough argued that spike protein presence in circulation may play a central role in clotting events across vaccine platforms.
Karl Jablonowski, a senior research scientist with CHD, said the discovery highlights gaps in scientific understanding of vaccine-immune interactions, emphasizing that the findings apply specifically to adenovirus-vectored vaccines rather than mRNA or other vaccine technologies.
Internal medicine physician Dr. Clayton J. Baker noted that implicating adenoviral vector technology in VITT could strengthen arguments that mRNA platforms may offer safety advantages in this particular context.
Meanwhile, vaccine injury advocate Brianne Dressen, founder of React19, said her organization includes members who developed clotting complications after receiving both adenoviral vector and mRNA vaccines, maintaining that while rates differ, serious adverse events have been reported across platforms.
Researchers stress that VITT remains extremely rare relative to the number of doses administered worldwide.
Nonetheless, the newly identified immune pathway provides a clearer understanding of how the condition develops and may guide future vaccine design and safety monitoring.
As scientific debate continues, experts agree that the findings represent an important step in understanding rare immune-mediated complications linked to certain vaccine technologies.
Trending

 Education1 week ago
Education1 week agoWhy some UTME results are withheld, JAMB explains

 Business1 week ago
Business1 week agoZenith Bank breaks N5trn barrier, emerges Nigeria’s most valuable banking stock

 Agribusiness1 week ago
Agribusiness1 week agoInsecurity, rising costs push food prices higher

 Aviation6 days ago
Aviation6 days agoAirlines averted shutdown as FG approves debt relief, aviation tax review
 Health1 week ago
Health1 week agoU.S. COVID-19 vaccine injury program compensates few claims amid high denials

 Politics1 week ago
Politics1 week agoGov. Yusuf nominates Garo as Kano Deputy Governor amid political shift

 Energy1 week ago
Energy1 week agoOil windfall meets rising costs as Nigeria gains $4bn amid global energy shock

 Health5 days ago
Health5 days agoWorkplace stress driving global health crisis, ILO warns

